Non-coeliac gluten sensitivity (NCGS) presents with non-specific symptoms that occur both intestinally and extra-intestinally and resemble the symptoms of coeliac disease or wheat allergy. Diagnosis is made based on the response to a gluten-free diet, after coeliac disease and wheat allergy have been ruled out.
There is a group of patients who respond to the consumption of food containing gluten with symptoms such as abdominal pain, fatigue, headaches, rashes, or mental confusion ("foggy mind"). However, neither coeliac disease nor wheat allergy is present in these instances. When these patients avoid gluten, their symptoms improve within a few weeks; when they are re-exposed to gluten the symptoms return. Whether the gluten or some other component of wheat is actually responsible for the reactions is currently the subject of debate in the scientific community.
Since the original definition of NCGS by the Salerno Experts’ Criteria [1], it has been recognised that other components of wheat other than gluten proteins are potentially deleterious for NCGS patients, which include amylase/trypsin inhibitors (ATIs), wheat germ agglutenins (WGA) and fermentable oligo-, di- and monosaccharides and polyols (FODMAPs) [2]. For this reason, some experts in this field may refer to NCGS more broadly as non-coeliac wheat sensitivity (NCWS), with further research required to elucidate the causal agent.
Differences in comparison to coeliac disease and wheat allergy
All three gluten-related disorders - NCGS, coeliac disease and wheat allergy - have similar symptoms and are therefore easily confused. However, there are differences, e.g. in terms of reaction times and pathogenesis. Coeliac disease is an autoimmune enteropathy caused by gluten. Wheat allergy is an IgE-mediated response to wheat. Although people with NCGS develop symptoms similar to those observed in coeliac disease after eating food containing gluten, the clinical picture is generally less severe and it is not possible to determine auto-antibodies, anti-tissue-transglutaminases or autoimmune concomitant diseases. In contrast to coeliac disease patients, patients with NCGS exhibit little histological change or only lesions in the small intestine mucosa, which corresponds to 0 - 1 on the Marsh scale.
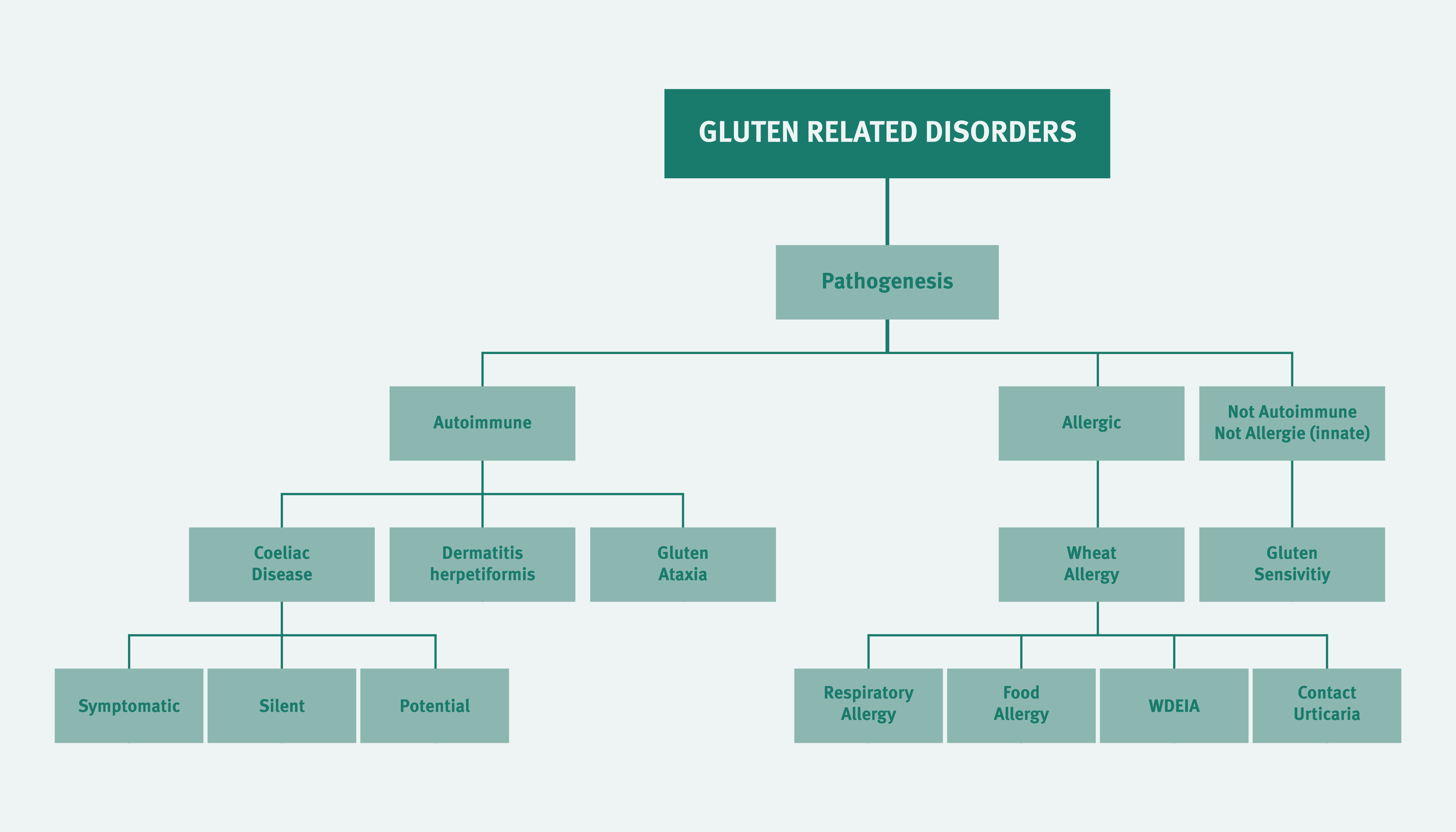
Overview of how to distinguish between coeliac disease, NCGS and wheat allergy
| Coeliac disease | Gluten sensitivity | Wheat allergy | |
| Period between exposure to gluten and onset of symptoms | Weeks to years | Hours to days | Immediate reaction: a few hours Delayed reaction: a few hours to two days |
| Pathogenesis | Autoimmune (congenital + adaptive immunity) |
Currently unclear immunological reaction | IgE formation and IgE-mediated mediator release |
| HLA | HLA DQ2/8 (approx. 95% of cases) |
Unclear | - |
| Autoantibodies | Positive (high sensitivity and specificity) |
Negative (except anti-gliadin antibodies IgA and/or IgG) |
Positive |
| Enteropathy | Typical | Missing; occasionally IEL slightly elevated (Marsh 0-1) |
Missing |
| Symptoms | Intestinal and extra-intestinal | Intestinal and extra-intestinal | Intestinal and extra-intestinal |
| Complications | Concomitant diseases, long-term complications | No concomitant diseases, long-term complications unknown | No concomitant diseases |
| Therapy | Long-term implementation of a gluten-free diet is necessary Persons with coeliac disease may must avoid foods containing gluten, even those that contain only traces of gluten, for their entire life |
The minimum time frame should be no less than one or two years The minimum time frame should be no less than one or two years The tolerance threshold of patients with NCGS varies, i.e. gluten intake must be adjusted individually |
Temporary avoidance of wheat-based foods is sometimes sufficient Administration of cortisone may be necessary |
References
- Catassi C, Elli L, Bonaz, B, Bouma, G, et al. Diagnosis of non-celiac gluten sensitivity (NCGS): The salerno experts’ criteria. Nutrients 2015, 7, 4966–4977
- Catassi C, Alaedini A, Bojarski et al. The Overlapping Area of Non-Celiac Gluten Sensitivity (NCGS) and Wheat-Sensitive Irritable Bowel Syndrome (IBS): An Update . Nutrients 2017, 9, 1268
